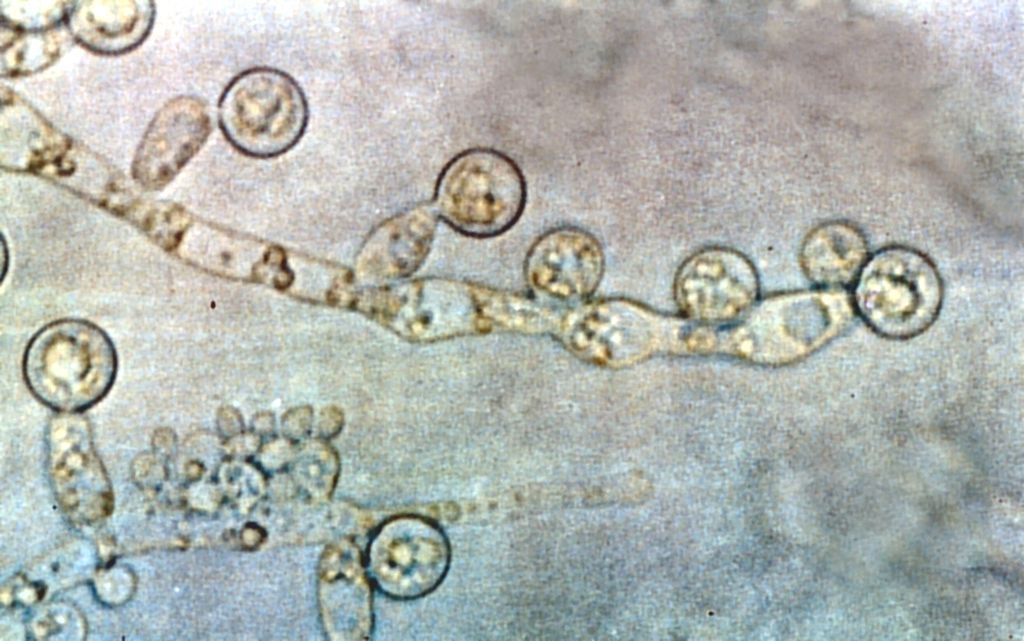
A new research from scientists at Weill Cornell Medicine has found that the common fungi present in the gut teaches the immune system on ways to respond to their more dangerous relatives.
The study revealed the complex relationship between humans and their associated microbes. It also has shown ways that could help combat a rising tide of drug-resistant pathogens.
They made the discovery from information based on inflammatory bowel disease, which is often affiliated to people carrying more than normal amounts of fungi in their guts.
These patients develop strong antibody responses against mannan, Mannan is a molecule which is common in a wide range of fungal species.
Dr.Iliyan Iliev, associate professor of immunology in medicine in the Division of Gastroenterology and Hepatology at Weill Cornell Medicine, found that healthy controls in these studies had shown some level of anti-fungal bodies.
Dr. Iliev added that there was no proof for fungal infections in healthy individuals they examined. So they focused on the function of the antibodies.
The research team developed a platform which allows them to determine which gut fungi was getting targeted by antibodies in blood of individual patients.
A strong response was found against the yeast Candida albicans.
Experiments in mice by Dr. Iliev and Itai Doron, lead author of the study, found that even though the animal’s guts didn’t develop blood-borne fungal infections colonizing the animals’ guts with Candida albicans caused them to develop antibodies against the fungus in their bloodstreams.
The animal’s immune cells seemed to transport fungal antigens to the spleen, stimulating the production of circulating antibodies in the bloodstream. “Those fungi just educate that immune response,” Dr. Iliev said.
The fungi in the gut can invade bloodstream and cause life-threatening infections in case of patients with suppressed immune systems. The team mimicked this process by treating mice with immunosuppressive drugs.
They found that the candida species on colonizing the gut of the mice, allowed the fungus to move into the bloodstream causing fatal infections. The immunosuppressed mice when treated with purified anti-fungal antibodies from donor animals were protected from these infections.
The same idea worked out in case of infections with either Candida albicans or the emerging pathogenic yeast Candida auris. These have become a major issue of concern in immunosuppressed patients and the elderly in recent years.
In collaboration with researchers at INSERM in Paris, France, the team also looked at serum from patients with mutations in a gene called CARD9.
This mutation affects a critical adapter protein in the immune system, leaving the affected individuals susceptible to severe fungal infections.
Besides this, the team also added that they found the serum of these patients lacked anti-fungal antibodies normally seen in serum of patients without mutation. The experiments have confirmed the important role of CARD9 in priming the production of antifungal antibodies.
The result was that normal intestinal fungi like Candida albicans could potentially be functioning as a kind of intestinal vaccine against this fungal infection in healthy people by inducing the production of blood-borne antibodies that can target multiple species of potentially pathogenic fungi. The antibodies bind and destroy the fungi once they enter the bloodstream.
Whereas patients with lower immunity are more susceptible to this fungal infection. New therapies that involve either stimulating the production of anti-fungal antibodies, or injecting such purified antibodies directly into patients’ bloodstreams, might help combat these increasingly common infections.
“Many fungal infections in immunosuppressed patients and elderly patients are happening by translocation of pathogenic Candida species from the gastrointestinal tract, and the survival rates upon systemic spreading are alarmingly low,” said Dr.Iliev.
Journal Reference:
Itai Doron et al. Human gut mycobiota tune immunity via CARD9-dependent induction of anti-fungal IgG antibodies, Cell (2021). DOI: 10.1016/j.cell.2021.01.016