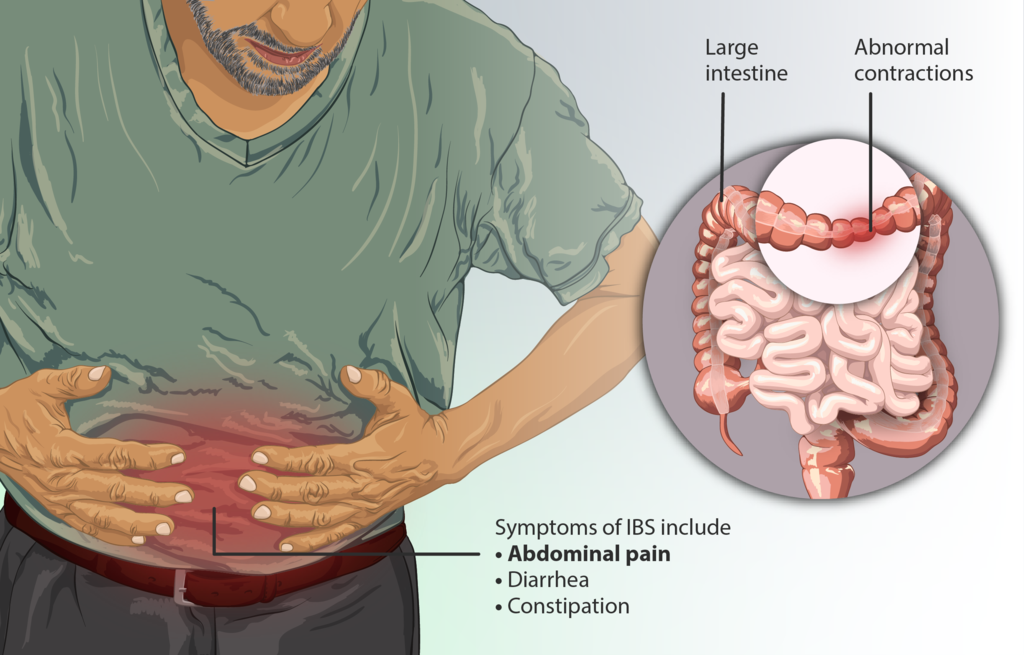
A new research by KU Leuven researchers has found out the biological mechanism that explains why some people experience abdominal pain when they eat certain foods. This finding now paves way for more efficient treatment of what is called the irritable bowel syndrome and other food intolerances.
Statistics show that around 20% of the world’s population suffers from irritable bowel syndrome (IBS), which causes stomach pain or severe discomfort after eating. This also affects their quality of life. Some diets like gluten-free ones can help in giving some relief, but the reason this works is still unknown. The patients are not allergic to foods, nor they have known conditions such as coeliac disease.
Professor Guy Boeckxstaens, a gastroenterologist at KU Leuven and lead author of the new research, said that these patients aren’t taken on a serious note by the physicians and the lack of an allergic response is used as an argument for saying that there is no problem in patients gut physiology.
New insights help us provide more light on the fact that we are dealing with a real disease.
The studies have revealed a mechanism that connects certain foods with activation of the cells that release histamine (called mast cells), and subsequent pain and discomfort.
The work by Professor Boeckxstaens has shown that blocking histamine improves the condition of the people with IBS.
In case of a healthy intestine, the immune system doesn’t react to foods so the first step was to find out what could cause such a tolerance to breakdown.
Since people with IBS often report that their symptoms began after a gastrointestinal infection, such as food poisoning, the researchers started with the idea that an infection, while a particular food is present in the gut, might sensitise the immune system to that food.
They infected mice with a stomach bug, and at the same time fed them ovalbumin, a protein found in egg white that is commonly used in experiments as a model food antigen.
Once the infection is cleared, they would again give the mice ovalbumin in-order to check if the immune system of the mice became sensitive to it. The result was positive,
The ovalbumin on its own provoked mast cell activation, histamine release, and digestive intolerance with increased abdominal pain. This was not the case in mice that had not been infected with the bug and received ovalbumin.
The researchers could then unpick the series of events in immune response that connected the ingestion of ovalbumin to activation of the mast cells. It was found that this immune response occurred in the part of the intestine infected by disruptive bacteria. There were no general symptoms of food allergy.
Boeckxstaens speculates that this points to a spectrum of food-related immune diseases.
One end of the spectrum is an immune response to a food antigen such as in IBS and at the other end, it is a food allergy, comprising a generalised condition of severe mast cell activation, with an impact on breathing, blood pressure, and so on.
After the research on mice, they now studied it on humans. The reaction was similar to that of mice. The small number of people involved makes it in need of more information to confirm the facts. A larger trial is on the way and we hope to get the best of it concluded.
Journal Reference:
Aguilera-Lizarraga, J., Florens, M.V., Viola, M.F. et al. Local immune response to food antigens drives meal-induced abdominal pain. Nature (2021). DOI: 10.1038/s41586-020-03118-2
Press Release: KU Leuven